Monday 11/11/2019 – Saturday 11/16/2019: ICU
I was in the ICU for a total of nine days while they kept my blood pressure very tightly controlled and checked me daily for vasospasms. (They got a concerning doppler reading one time, so off I went with Substitute Charlee for another CT scan; it did show vasospasms were occurring, but I remained asymptomatic, and scanned clean the next day.) My cousins and a few friends continued to drop by to keep me company, which was nice, and I had a series of terrific ICU nurses to take care of me. After a few days in ICU they decided to take out my IV and put in a subclavian PICC line, so they could administer medications and draw blood without having to stick me all the time. That was a relief, although the process of getting it put in was far from fun. Once the PICC line was there I mostly forgot about it; funny what you can get used to when you have to, and when the alternative is multiple jabs with sharp pointy objects.
In the immediate aftermath of The Event my body temperature had been fluctuating widely; the spiking temperatures, up into the 102-103 range, were frequently accompanied by full body sweats, which felt a lot like the sweat that had occurred when my aneurysm had ruptured. The first time such a spike happened, the friend who was with me—who is always warm—immediately summoned a nurse, because, as he later explained it to me:
Friend #2: “Your forehead felt hot, and nobody’s forehead ever feels hot to me.”
The nurse came and checked me out and explained that they usually saw these sort of temperature irregularities in subarchnoid hemorrhage patients, because the brain’s regulating systems have gotten out of whack.
Nurse #1: “I’ve seen temperatures as high as 107 degrees with no infection.”
At that point I was already on acetaminophen for pain—I couldn’t have narcotics for quite a while after The Event—and that’s also a fever reducer, so it helped keep things under control. My temperature never got as high as 107, as far as I know, but the spikes continued the entire time I was in the hospital and for several weeks after I got home. (After I was released, this almost caused me to ignore a fever that turned out to be a nosocomial infection, but more on that later.)
This wasn’t the only symptom that persisted throughout my hospital stay. Others included an extreme light sensitivity (I was forever asking people to turn the lights off) and an inability to read or look at screens. No television or tablet time for me in ICU! I also had a very stiff neck for a long time, and a pretty bad headache, unsurprisingly, for the first week or so. But as I told my wife, by the Monday following The Event, I was starting to feel human again. Which meant I started to notice things like my teeth hadn’t been brushed in a while and my beard was getting annoyingly shaggy. The hospital supplied a toothbrush and toothpaste, and I asked my wife to start bringing in my shaver from home.
Nurse #1: “Good idea. You don’t want to use our razors. The blades are awful.”
So most mornings, after breakfast, I would brush my teeth and shave just like at home, except I was doing it in bed, connected to a bunch of wires, tubes, and machines, and with medical staff coming and going. One time a beeping machine brought a random nurse in to check on it while I was shaving.
Random Nurse (watching me shave): “You look pretty good. What are you even doing here?”
Me: “I’m squatting. It’s cheaper than rent in San Diego.”
Random Nurse (snorting): “Oh I doubt that.”*
Speaking of breakfast, the first several days, it just appeared, on trays bearing foods that had been selected by … someone? I guess there’s a default breakfast that you get if you haven’t filled out menu selections. This default breakfast always included a cup of coffee, which I refrained from drinking, on the theory that I probably shouldn’t be drinking caffeine right then. (Sure enough, when menus did start appearing early in the week, coffee and tea and any other form of caffeine was always crossed out.)
Tuesday or Wednesday, I finally got some heavier-duty painkillers. As I mentioned, for the first several days the only thing they would give me was acetaminophen, because narcotics would interfere with the neurological tests they were doing. During this time I consistently reported headaches in the range of 2-4 on the pain scale, after which I would always have to explain that my pain scale goes from 0 to kidney stones. Having kidney stones on the board seriously screws up the pain curve.
Nurse #3: “What would you rate your headache pain at?”
Me (eyes closed, rubbing forehead and temples): “Maybe a three.”
Nurse #3 (using her dubious voice): “That doesn’t look like a three to me.”
Eventually it was decided that next time I’m in the hospital** I will use a pain scale that is only for the part that actually hurts and does not include kidney stones (unless of course I’m there for another kidney stone)—so in this case it would maybe be 0 to migraine—but I didn’t want to change the scale mid-treatment and suddenly double or triple my pain level and really freak everybody out. Anyway it wasn’t like I didn’t get acetaminophen as often as permitted; and when I was finally approved for something stronger, they immediately put me on Norco, which was considerably more effective. Unfortunately, as they warned me at the time, Norco (and narcotics in general) can really plug you up, which is a bad thing when you’ve only recently gone back on solid food, and the last time you had a bowel movement it landed you in the emergency room with a ruptured aneurysm. It didn’t help that it was nearly a week before I was allowed to even sit up in bed.
Nurse #1: “Sorry, they’re being very cautious with you.”
Me: “I understand, nobody wants to mess up their success story. Yeah, he was doing great until he fell out of bed trying to go to the bathroom and fractured his skull.“
So there I was plugged up by the Norco, trying to use the bed pan, without doing any straining. The fiber and stool softeners they had been giving me were wholly inadequate to the task at hand; and besides, pooping in bed is not what one does. I did try several times but the final tally was Mom’s Training 3, Bedpan 0.
Nurse #2: “Any bowel movement yet?”
Me: “Not yet.”
Nurse #2: “Are you passing gas?”
Me: “Oh yeah. I’m not even being subtle about it.”
Nurse #2: “Good. No, that’s good. We like all that stuff. We just don’t like the dinner guest.”
I did have another visit from the “dinner guest” during the week; one afternoon, while talking to Cousin #2, I out of nowhere vomited up something that (mostly) looked like the previous night’s supper.
Me: “That’s not good.”
Vomiting after you’ve had a brain injury is a sure way to bring the nurses and doctors running.
Nurse #2: “Uh-oh, what happened?”
Cousin #2: “We were talking and he just suddenly threw up. He said it looks like last night’s dinner.”
Me: “At least the coffee cake was covered up.”***
Nurse #2 (to cousin, sounding relieved): “Well, he still seems to be sharp as a tack.”
After that I got a visit from every doctor I had seen so far, but the ultimate consensus was that it was a one-off and not something we needed to worry about. Evidently the veggie lasagna dinner from the night before didn’t agree with me, although Nurse #2 had his own theory.
Nurse #2: “I think it was your pants.”
The pants in question can be seen below, in the clip of my physical therapy. Did they make me throw up? Well, they are pretty busy and colorful, but considering that I went to the hospital in vomit-covered clothes, I was grateful to have them. (Cousin #2 had picked them up and brought them for me, along with several other pairs of pants that were not quite as, shall we say, festive.)
Speaking of throwing up, during the week, I got to meet a nurse who had helped take care of me when I was first in ICU.
Nurse #1: “Hey, do you remember Other Nurse? She was here when they brought you in. We were getting you into bed when you started vomiting, and she helped us get you upright so you wouldn’t aspirate. She told you to turn your head and you turned towards her and vomited all over her. She was asking how you were doing and wants to come see you.”
I didn’t really remember Other Nurse, but I did vaguely remember throwing up while lying down, not being able to clear it from my mouth, and thinking, This is bad. But at the time I was semiconscious at best. Anyway, a little later, Nurse #1 and Other Nurse came in for a brief visit.
Other Nurse: “How are you? Oh you look so much better than when you came in.”
Me: “Thank you. I hear I owe you an apology.”
Other Nurse: “No no, it happens all the time.”
Later on I mentioned this incident to Friend #4.
Me: “Yeah, I guess I threw up all over her. See, that’s the reason I could never be a nurse.”
Friend #4: “That’s the only reason, huh?”
Me: “Well, that, and the needles, and the blood and … Well there are lots of reasons.”
Towards the middle of the week, Nurse #1 got them to approve a bedside commode. But I was still having trouble, due to the fact that by now I was on Norco, which is a heavier duty painkiller and also, oddly enough, a city in California. So eventually additional assistance was required, if you know what I mean.
Nurse #2: “I call this pocket dynamite.”
Not long thereafter, we were ready to go.
Nurse #2: “Should I get you a magazine?”
Me: “Do you have a magazine?”
Nurse #2: “Uh, I think I have a catalogue or something …”
Once again it was Nurse #1 to the rescue. She dashed in a few minutes later with a copy of Esquire. I don’t know where she found the magazine, but I read all about Jason Momoa’s dogs while business was getting done.
Another elimination problem was that I still needed my catheter, because that side of the system was plugged up too. I could go a little, but there was a definite retention problem, and so after taking the catheter out, they had to put it back in a day or two later. (This happened twice and then they decided to just leave it.) One of the nurses theorized that there had been a little bit of damage done when the catheter was inserted in such a hurry during my sojourn in the emergency room (I told you that was going to come back to bite me) but nobody really can say for sure.
Because I was more or less confined to bed and not being allowed to walk around freely, I spent my entire time in the hospital with Intermittent Pneumatic Compression Devices on my lower legs. These are wraps connected to air hoses (more tubes!) that alternate squeezing both calves to keep blood in the veins flowing back to the heart and thus avoid clots, because the last thing you need when you’re in ICU is an extra blood clot or two. In order for me to get up and use the portable commode, these needed to be disconnected and removed, which was usually done by a nurse. (I had to call a nurse anyway whenever I wanted to get up, because otherwise an alarm would go off somewhere that the ward had an escapee. ICU beds are rigged up with more traps than a tomb that’s being explored by Indiana Jones.)
Me: “I need my leg thingies hooked back up. I don’t know what their real name is.”
Random Nurse: “Most people just call them ‘squeezers’.”
Me: “Okay. I’ve been thinking of them as ‘vizslas’ because when they squeeze they remind me of the dogs we used to have that liked to lie on my legs, but I figured nobody would know what I was talking about if I said that.”
Cousin #2: “Maybe that means Tucker and Dennis are here keeping you company.”
So that was a nice thought. I held onto that one for the whole time I was hospitalized.
Towards the end of the week, with the assistance of a physical therapist, I did get to remove the “vizslas” and start taking walks around the ICU. Surveying my domain, if you will. I got to see some of my nurses out in their natural habitat, and met another nurse who had been in attendance when I was brought in, but who hadn’t gotten assigned to my room since then. She was quite happy that I was out and about.
Random Nurse: “Oh it’s good to see you walking. You look so much better. You were so sick, and your poor wife was so scared.”
The physical therapy didn’t just involve walking. It involved silly walks. These included things like flicking your heels up and smacking them with your opposite hand, crab-walking sideways, and something very much like what John Cleese does in the classic Monty Python skit. Not that I could possibly high-kick like John Cleese did.
But my favorite moment from our little jaunts around ICU was when the physical therapist said she wanted me to do a grapevine.
Me: “Ooh! The grapevine? I do those all the time!”****
And so we did the grapevine:
Those are the pants Nurse #2 blamed for the vomiting incident. I hope they didn’t make any of you throw up. (I’ve still been wearing them at home as pajama bottoms. Still have those hospital-issued slipper socks, too. Fashion for miles.)
I’ve mentioned the neurological evaluations few times. One of them involves looking at a picture and describing what’s happening in it. I was getting pretty bored in the hospital, so I started to prepare stories ahead of time to answer the question of “What’s going on in this picture?”
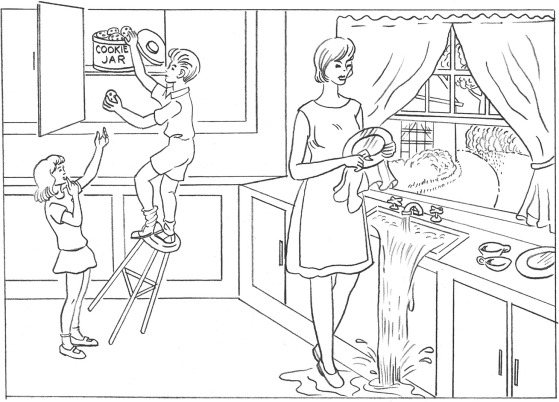 The first few times I simply described it, but what fun is that? I don’t remember all the scenarios I came up with (I mean, some of them were at like 1am) but here’s a sampling:
The first few times I simply described it, but what fun is that? I don’t remember all the scenarios I came up with (I mean, some of them were at like 1am) but here’s a sampling:
- “Mary is wondering why Ted still isn’t home from work yet. She’s not going to keep making dinner every night if he can’t bother to come home. Meanwhile, the kids are stealing cookies behind her back, but they’re being careless, and Tommy’s going to crack his skull on the counter and end up here in ICU.”
- “Sue couldn’t believe the neighbor was mowing the lawn naked again. She was definitely going to call the cops on him this time. Meanwhile, the kids are stealing cookies behind her back, but they’re being careless, and Tommy’s going to crack his skull on the counter and end up here in ICU.”
- “The kids thought it would be funny to switch Mom’s stash with the oregano in the spice cabinet, and now look what happened after she made spaghetti sauce. She’s spacing out at the sink and the kids have a serious case of the munchies and are stealing cookies, but they’re being careless, and Tommy’s going to crack his skull on the counter and end up here in ICU.”
Sucked to be Tommy, I tell you what.
One other interesting feature about my ICU room was that the bathroom had a very large window, which let in such a huge amount of light that it hurt my times every time anyone opened the door to it. And, apparently it got very, very hot during the day.
Friend #2: “That room is like a sauna.”
Me: “So I’ve heard. I haven’t been in it. I have yet to explore all the rooms of my mansion.”
This led to an interesting movie-related discussion (as an old coworker noted, everything reminds me either of a Simpsons episode or a movie):
Me: “Every time somebody opens that door it’s like looking into the trunk of the car in Pulp Fiction.”
Nurse #1: “I know! Hey, what do you think was in the trunk of that car, anyway?”
(a discussion of what we think might have been in the trunk of the car ensues)
Me (turning to Friend #3, who was visiting at the time): “What do you think was in the trunk of the car?”
Friend #3: “I never actually saw Pulp Fiction.”
(all conversation ceases as Nurse #1 and I both stare at Friend #3 as if she had suddenly sprouted a few extra heads)
Me (after a moment): “You could practically hear the needle scratching across the record there, couldn’t you?”
Towards the end of the week, we started hearing rumors that they thought I was doing well enough to be transferred out of ICU to a “step-down” unit, Telemetry. That weekend, these rumors were confirmed to be true; my wall hangings, blankets, pillow, and myself were all bundled up into a wheelchair and driven to our new hangout in a different wing of a hospital. So much like we never find out what’s in the trunk of the car in Pulp Fiction, I never found out what it was like to use the sauna-bathroom in ICU.
I didn’t have a whole lot of luck with the bathroom in Telemetry, either, but that’s a story for next time.
* Rents in San Diego are probably not as expensive as a room in ICU. Probably.
** I had saved the coffee cake from breakfast in a plastic shell that Cousin #1 had used to bring me doughnuts the previous day.
*** Hopefully never
**** Dances in which I do grapevines all the time include Foxtrot, Argentine tango, Nightclub Two-Step, and Quickstep.



So sorry to hear about this. Glad to see you keeping a sense of humor about it all though. Take care and get well soon!
LikeLiked by 1 person
Such adventures in the ICU! But perhaps it’s good you identify with Tommy and not Spacey Sue
LikeLiked by 1 person
So you’re a ballroom dancer!? We do grapevine all the time in foxtrot. Two young teenagers who were taking lessons from us met us at a dance, and saw us do that. The next waltz, they did the grapevine. We were too amazed to see them able to do that to a waltz to say don’t do that!
LikeLiked by 1 person
Yep, we’ve been taking ballroom lessons since 2001. I never suspected it would come in handy for physical therapy after a subarachnoid hemorrhage!
LikeLiked by 2 people
Ballroom dancing is definitely good for many things, LOL! It’s also top rated for keeping alzheimers at bay.
LikeLike
Oh, MY! Your humor is just what I needed today, after a crazy shift at the nursing facility where I work…and I loved your descriptive renderings of your stay in ICU.
I shall have to remember the Grapevine moves, next time I help someone ambulate in the hallways, LOL!
Thanks for sharing your story with all of us:)
LikeLike
Oh James your ordeal was so other wordly!! How you maintained a sense of humour I’ve no idea but you are a trooper! Now about silly walks I could not resist “Don’t Mention The war” with John Cleese. I hope I do not offend…I am Jewish & find this sketch hilarious so please accept it in the humor it is meant!
An no wonder you were vomiting; those pants are something else!! ROFWL!!
My favorite line was when you told the Nurse you were squatting as it was cheaper than rent!! I choked on my tea laughing so hard!!!
All I can say is I am so relieved & glad you made it thru & are here with all of us today!
{{{hugs}}} Sherri-Ellen & POTP BellaDharma
LikeLike
Glad you kept your sense of humor throughout- that helps aid in healing. You sure went through a lot.
LikeLike
I must say, your journey through the halls of medicine was most amazing.
LikeLike
Laughter keeps you strong, my friend. And it was nice to see you smiling for the grapevine. I also hate those leg squeezers. Had my experience with them last year. Got no sleep from the noise.
LikeLike
Loved watching the ‘grapevine’. You looked like a pro!
And absolutely loved your sense of humour; without it life could have been intolerable.
Well done you.
LikeLike
Were you wearing the pants at the time of “the event”? I think that might explain a lot. (And glad you’re well now, or at least well enough for us to talk smack about it.)
LikeLike
Not at the time of The Event, but I was wearing them when I threw up (almost) all over my cousin! 😀
LikeLiked by 1 person
Btw, thanks for including the silly walks clip. 🙂
LikeLike